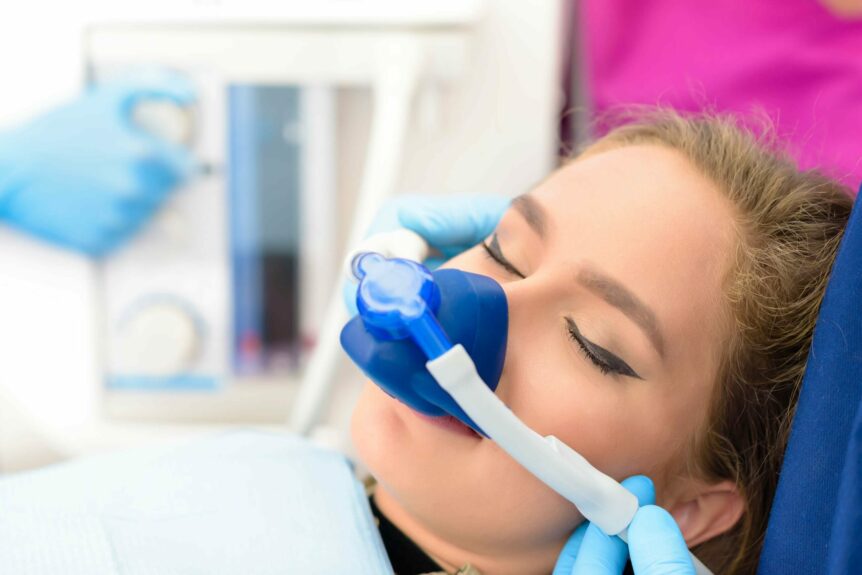
What is Sedation Dentistry?
Conscious sedation dentistry involves the administration of sedative drugs to reduce anxiety before dental procedures. Patients take the drugs orally, intravenously (IV), or through inhalation (nitrous oxide). Sedation dentists generally administer sedatives to those who suffer from dental phobia, generalized anxiety, belonephobia (fear of needles), or previous dental trauma. Patients with high anxiety levels may be sedated before receiving an injection of anesthesia (pain control medicine), especially if they have a fear of needles.
Anxiety vs Dental Phobia
Anxiety or fear of receiving dental treatment is not uncommon and affects about three-fourths of the American population. About five to ten percent of people experience dental phobia (also called dental fear, dental anxiety, or dentophobia)
By definition, dental phobia is the intense fear of visiting the dentist. Sedation dentistry is the ideal option for those with dentophobia. Those with minor fears and anxieties about dental treatment do not typically need sedatives.
Understanding Dentophobia
The definition of “phobia” is something that is:
- Irrational to the demands of the situation
- Beyond voluntary control
- Inexplainable
- Persistent long-term
- Not age-specific
In particular, dental phobia develops over time and may be related to previous traumatic dental experiences, outside influences, childhood anxiety, and the dental office environment in general.
Childhood Anxiety and Fears — Dentophobia is a function of personality development that is associated with feelings of abandonment and helplessness. If a child grows up with anxiety and continues to experience it into adulthood, they are more likely to develop phobias.
Sufferers of dental anxiety also typically find the smells, sounds (such as drills), and sights of dental surgery overwhelming. In some cases, simply seeing a dentist in a white coat can trigger dental anxiety.
Dental fears can even be associated with extreme childhood fears. These fears may include the dark, thunder, certain animals, imaginary figures, or being alone in a dentist’s chair as a child.
Traumatic Dental Experiences — Frightening, embarrassing, or painful dental experiences are the primary causes of dental anxiety, especially in children. If a patient had a negative experience with a dentist in the past, they may end up mistrusting all dentists.
Dental Office Environment — Dental anxiety can be induced by just thinking about a dentist visit or by actually experiencing one. This may include:
- Anesthesia injections, needles, or sharp objects.
- The sound of dental drills, tools, and scraping of the teeth.
- The dentist’s mannerisms, attitude, and personality.
- Fear of criticism by the dentist.
Outside Influences — Hearing negative comments about dentistry can induce fears about treatment from a young age. This can also increase dental anxiety over time and often results in unpleasant experiences.
Common Types of Sedatives used in Sedation Dentistry
Sedation dentists determine which sedation is best for each patient based on the procedure type (invasive or minor), the patient’s preference, and their medical history. There are three main types of sedation, including:
Laughing Gas
Laughing gas (anxiolytic) consists of nitrous oxide that patients receive through inhalation. Combining local anesthesia and laughing gas during dental procedures reduces feelings of anxiety, pain, and fear.
Laughing gas is a form of conscious sedation, which means it does not put patients to sleep. The effects of nitrous oxide are almost instant after the mask is placed (about 30 seconds). The sedative wears off quickly after the patient breathes oxygen. Patients on nitrous have to breathe 100 percent oxygen for five minutes before removing the mask.
Oral Sedation
Oral sedation is a “premedication.” Patients take this type of sedative before a surgical or invasive dental procedure. The premedication offers a safe approach to sedation that is not administered through an injection. It is more potent than inhalation sedation (laughing gas). It requires less co-operation between dentist and patient because patients often fall asleep after receiving oral sedation medications.
These sedatives help manage anxious patients under conscious sedation and may be taken:
- The night before the procedure to help reduce anxiety.
- One to two hours before treatment to help reduce anxiety.
- Before a needle is administered (for those who are needle phobic).
IV Sedation
IV sedation, also referred to as deep sedation, is a conscious form of sedation. The drug makes patients very sleepy and almost completely unaware of their surroundings. Dentists use this type of sedation during oral surgeries.
Common surgeries include wisdom teeth removal, extractions, root canal treatment, and gum disease treatment.
Most patients do not remember anything during the procedure but remain completely conscious. The dentist can also easily wake patients up at any time. Modern IV sedatives consist of benzodiazepines, such as diazepam or valium. The drugs act in the central nervous system to reduce anxiety and produce hypnotic sensations. An IV sedation acts very quickly after administration and the effects can last for a few hours after treatment is complete.
Benefits of Sedation Dentistry
Those with dentophobia typically refrain from visiting dentists at all. Neglecting the dentist results in a higher chance of developing gum disease, cavities, and other serious oral conditions.
With sedation dentistry, more people are able to visit the dentist with less uncontrollable fears and anxieties about treatment. Long and complex procedures typically incorporate sedatives, which may benefit people who have:
- Dental phobia
- Extreme anxiety or fear of needles
- Sensitive teeth
- Sensitive gag reflexes
- Low pain thresholds
3 Possible Side Effects of Sedatives
Sedation dentistry is a common and safe treatment. Before administration, the dentist should be aware of the patient’s full medical history and any allergies to ensure complications are avoided. Side effects are rare, but may include:
- Nausea (before or post-procedure)
- Drowsiness or sleepiness (post-procedure)
- Dizziness (before or post-procedure)